Why Do Pediatricians Not Recommend the Owlet Smart Sock — and What to Use Instead?
- Created:
3. 3. 2026 - Updated:
2. 3. 2026
If you’ve ever stared at your sleeping newborn and thought, “Are they breathing?” — you’re not alone. That exact fear is why products like the Owlet Sock have become so popular. A wearable “smart sock” that tracks oxygen and heart rate sounds like an ultimate peace-of-mind purchase.
But when you ask many paediatricians about consumer wearables like the Owlet Sock, you’ll often hear a version of: “It’s not recommended for healthy babies as a way to prevent SIDS — and it can create new problems.” That doesn’t mean you’re a bad parent for thinking about it. It means the why behind the recommendation matters — andthere are safer, simpler (and often cheaper) ways to get the reassurance most parents are really looking for.
Below is what major pediatric and medical sources say, the practical reasons doctors hesitate, and what you can use instead — without strapping anything to your baby.
The Key Misunderstanding: Owlet Isn’t a “SIDS Prevention” Tool
A lot of the Owlet Sock’s appeal is emotional: it feels like an extra layer of protection against the scariest “what if.” The problem is that no consumer monitor has been shown to prevent SIDS — and the American Academy of Pediatrics (AAP) is explicit about that.
In the AAP’s 2022 safe sleep policy statement (the backbone of many pediatricians’ guidance), the recommendation is explicit: “Do not use home cardiorespiratory monitors as a strategy to reduce the risk of SIDS.”
HealthyChildren.org (AAP’s parent-focused site) repeats this in plain language and warns against letting monitors create a false sense of security.
In a nutshell: the AAP isn’t saying “never use any baby monitor.” It’s saying don’t buy a wearable vital-sign monitor expecting it to reduce SIDS risk, and don’t let it replace proven safe-sleep practices.
Why Pediatricians Often Say “Skip It” for Healthy Babies
Reason A: For healthy infants, it’s usually unnecessary medicalization
Children’s Hospital of Philadelphia (CHOP) summarizes the clinical perspective bluntly: it’s not necessary to monitor vital signs of healthy infants at home, and it can create downstream harm.
The AAP also notes that many direct-to-consumer heart rate and pulse-ox devices historically fell under “wellness” positioning and, crucially, are not intended to prevent sleep-related deaths (even if the marketing vibes suggest otherwise).

Reason B: False alarms (and missed events) can do real damage
One of the biggest pediatric concerns isn’t just “it won’t help.” It’s it might create avoidable panic.
A well-known CHOP-led study published in JAMA compared consumer baby pulse-ox monitors (including an Owlet Smart Sock model) to an FDA-cleared hospital reference monitor. The Owlet detected hypoxemia but not consistently; and another consumer monitor in the study performed very poorly.
CHOP’s parent guidance highlights what happens in real life after false positives: families rush to the ER, babies may get unnecessary tests or admissions, and anxiety spikes.
Reason C: It can increase anxiety (or shift it into “alarm vigilance”)
Mayo Clinic’s parent education piece puts it clearly: home cardiorespiratory monitors (including Owlet-style devices) do not reduce SIDS risk, and frequent false alarms can raise parental anxiety.
The AAP also warns that these products may cause complacency with safe sleep — the exact opposite of what you want.
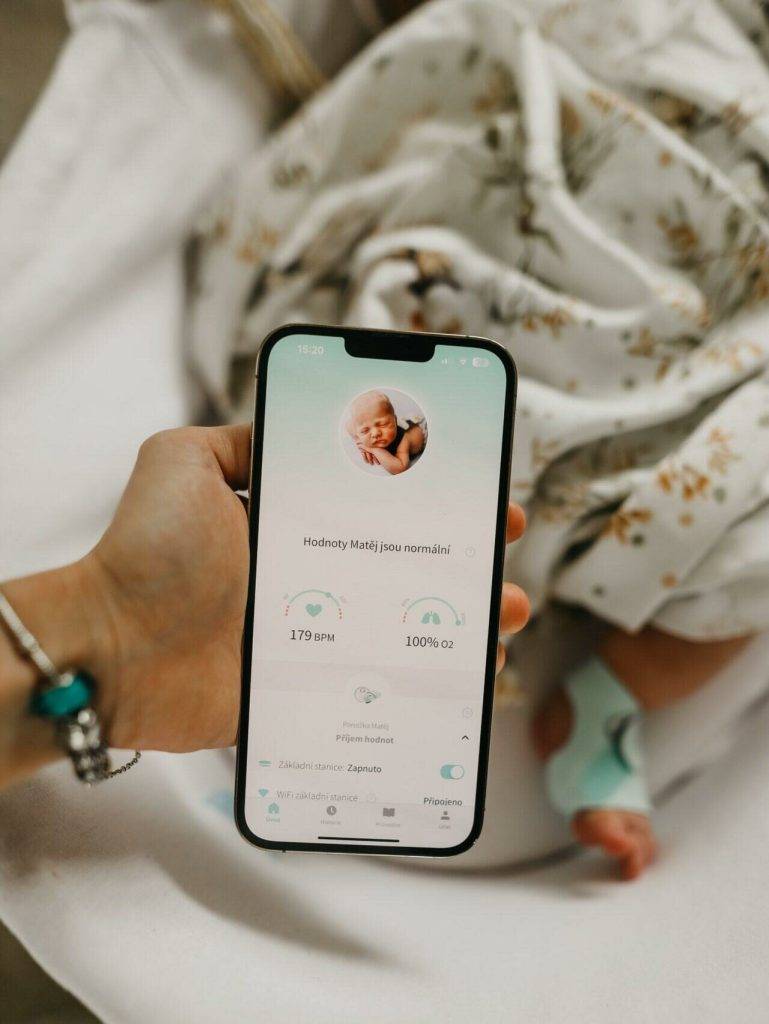
Reason D: Wearables add physical downsides you don’t get with a camera monitor
Any wearable worn for hours can cause skin issues. Owlet’s own help documentation includes detailed guidance about red marks, pressure injuries, friction, and skin irritation, plus recommendations as checking skin frequently and alternating feet.
That doesn’t mean every baby will have irritation — but it’s a risk that simply doesn’t exist with non-contact monitoring.
Reason E: Cost-to-benefit often doesn’t pencil out
Owlet’s Dream Sock is usually priced in the hundreds of dollars (Owlet lists a regular price of $299.99, sometimes discounted).
When pediatricians weigh “high cost + no proven SIDS prevention + potential false alarms,” many conclude: put that budget into proven safety and sanity upgrades: a safe sleep setup, postpartum support, or a reliable audio/video baby monitor.
Contemporary Pediatrics also flags cost as a practical concern and states that these devices should not replace safe sleep practices.
“But Isn’t Owlet Fda-Cleared Now?” Yes — and That Still Doesn’t Equal “Recommended for Sids Prevention.”
Owlet’s product landscape has changed over time:
- In 2021, the FDA issued a warning letter stating Owlet was marketing Smart Socks in the U.S. without required clearance/approval, based on how the product was promoted and used.
- Later, Owlet announced FDA pathways for newer devices. The American Academy of Sleep Medicine (AASM) reported that Owlet received De Novo clearance for the Dream Sock as an over-the-counter infant pulse oximetry solution, and also referenced BabySat as a prescription system for infants with medical conditions under physician supervision.
Here’s the important nuance parents deserve:
- FDA clearance can speak to performance/safety for a specific intended use (e.g., pulse oximetry).
- It does not mean “prevents SIDS.”
- And it does not override the AAP’s safe-sleep guidance that monitors are not a SIDS-reduction strategy.
So a pediatrician can simultaneously believe:
- a cleared pulse-ox can measure oxygen within stated accuracy parameters, and
- healthy babies generally don’t need that at home, and
- parents shouldn’t treat it like a protection against SIDS.
When Medical Monitoring Is Appropriate (And How Doctors Think About It)
There are babies who go home with medically indicated monitoring — for example, some premature infants with significant apnea history, babies on home oxygen, or infants with certain cardiopulmonary conditions.
CHOP emphasizes that for infants who truly need monitoring, there are hospital-grade devices prescribed by pediatricians, and families should have a plan for what alarms mean and what to do.
Mayo Clinic similarly notes that no home monitor prevents SIDS, but some medically complex infants may use monitoring under physician direction.
Bottom line: if your baby has a medical reason, your pediatrician will guide you toward the right device and thresholds. If your baby is healthy, most pediatricians prefer you focus on safe sleep + practical monitoring that helps you parent, not practice medicine.
What Most Parents Actually Want (And a Better Way to Get It)
If we strip away the marketing and get brutally honest, most parents aren’t looking to trend SpO₂ charts at 3 a.m.
They want to:
- hear the first cry or fuss,
- see whether baby is awake or just noisy-sleeping,
- check the room without tiptoeing in,
- feel confident enough to rest.
That is exactly what a high-quality baby monitor (audio/video + smart alerts) is for — and you can get that without a wearable.
If you still want Owlet-like “breathing reassurance,” look at camera-based options that avoid an electronic sock on your baby’s foot. Nanit pairs its camera with a Breathing Band (a patterned fabric band worn over sleepwear) so the camera can track breathing motion without sensors or electronics in the band.
Another alternative is Miku, which markets contact-free breathing and sleep tracking via its camera—no wearable required.
As with any consumer monitor, these should be viewed as convenience/reassurance tools—not a replacement for safe-sleep practices.
What to Use Instead: A Baby Monitor App (No Sock, No Sensor, No Skin Irritation)
Annie Baby Monitor App: Owlet-style peace of mind, without the wearable
If you want smart monitoring without attaching anything to your baby, the Annie Baby Monitor app is built for that use case.
It turns two devices you already have (phones/tablets/PCs) into a baby monitor — so you get real-time notifications and alerts without introducing vital-sign alarms that can cause panic in otherwise healthy babies.
Features parents actually use (and pediatricians don’t object to):
- HD video + audio monitoring
- Night vision so you can see baby without turning on lights
- Sound, cry and motion detection with smart notifications
- Two-way audio (talk back / soothe from another room)
- Lullabies and white noise for settling
- Sleep insights (tracking patterns without medicalizing your baby)
- Unlimited range using Wi-Fi or mobile data, and multi-device support
- No new equipment required (old phone/tablet works)

And because there’s no wearable, you automatically avoid:
- skin irritation / pressure marks / friction issues,
- the “is this alarm real?” spiral,
- and the temptation to treat consumer readings as a medical diagnosis.
The Real “Gold Standard”: Safe Sleep + a Practical Baby Monitor
There isn’t a gadget you can buy that “prevents SIDS.” In fact, the AAP explicitly says not to use home cardiorespiratory monitors as a strategy to reduce SIDS risk, and notes there’s no evidence consumer wearable/monitor devices decrease SIDS risk. The U.S. FDA is also blunt: no devices, including infant monitors, have been authorized to prevent SIDS/SUID.
Breathing/movement monitors can still have a role in clinical care (e.g., NICU monitoring of heart rate, breathing and oxygen for preterm or medically fragile babies), but that’s medical monitoring for medical conditions, not SIDS prevention.
In the Czech Republic, under-mattress breathing monitors like Nanny are used in some maternity wards and healthcare settings, and the manufacturer positions Nanny for both medical providers and home use—but it’s best thought of as an alarm, not a prevention tool.
In the UK and Australia, major safe-sleep organizations similarly emphasize that monitors may reassure parents but haven’t been shown to prevent SIDS/SUDI, so the “prevention tools” that actually work are the proven safe-sleep steps.
If you want the pediatrician-approved approach that actually reduces risk, it’s boring — and it works:
- back sleeping,
- firm, flat sleep surface,
- no soft bedding in the sleep space,
- smoke-free environment,
- room-sharing without bed-sharing (when possible),
- and consistent safe-sleep habits.
That’s what the AAP emphasizes — and it’s the reason SIDS rates dropped so significantly after major safe-sleep campaigns.
A baby monitor (like Annie Baby Monitor) fits cleanly into this: it helps you keep a constant eye on your baby, respond to baby’s needs without changing the sleep environment and without implying that a gadget can “prevent” the unpreventable.
Final Takeaway
Pediatricians don’t recommend Owlet-style socks for most healthy babies because:
- they’re not proven to reduce SIDS risk,
- they can cause false alarms, anxiety, and unnecessary medical visits,
- and wearables add skin/fit complications you don’t get with camera monitoring.
If what you want is practical reassurance — seeing and hearing your baby, getting smart alerts, monitoring sleep patterns — you can get that without a wearable.
Use a baby monitor. And if you want a flexible, travel-friendly option that doesn’t require buying new hardware, Annie Baby Monitor app is a good fit.
FAQ: Why Do Pediatricians Not Recommend the Owlet Smart Sock
Because major pediatric guidance says home vital-sign monitors shouldn’t be used to reduce SIDS risk, and they can create problems like false alarms, unnecessary medical visits, and increased parental anxiety.
For healthy babies, they’re generally unnecessary, don’t prevent SIDS, and can trigger stressful false alarms or lead parents to over-rely on a gadget instead of proven safe-sleep practices.
Most pediatricians do not recommend Owlet as a SIDS-risk-reduction tool; at best, some may view it as optional “reassurance tech” for certain families, but not medically necessary for healthy infants.
There’s no clinical evidence that Owlet (or any consumer monitor) prevents SIDS; the FDA also says no infant monitor is authorized to prevent SIDS/SUID.